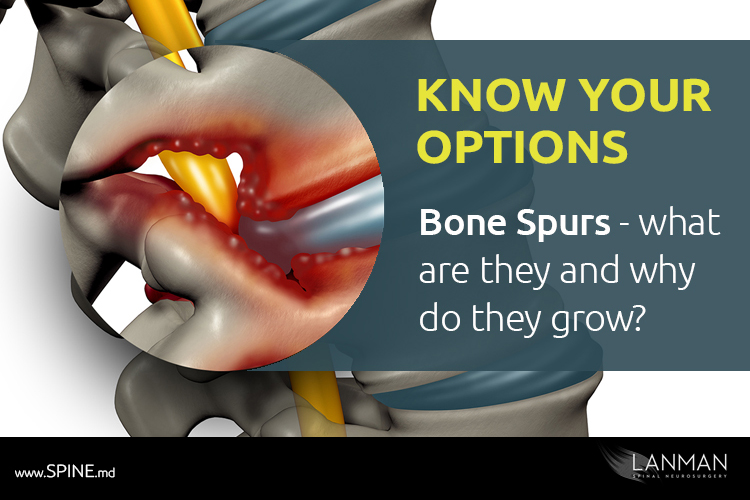
A bone spur is a nob of calcium that can grow along the edges of bones such as the vertebrae of the spine. The clinical name for them is osteophytes, or exostoses, both of which mean “bony projection.” The most common location where we find bone spurs is where bones meet each other.
The leading cause for bone spurs is joint damage such as osteoarthritis, untreated herniated or degenerated spinal disc, damage to tendons, or other joint damage.
Other patients who are at higher risk from bone spurs could be athletes. Overuse of joints or repetition movement raises the risk due to physically intense movements over a long period of time. Genes often have the most significant role in the development of spurs; if your parents had them, you’d probably develop them too. Other factors that can lead to this condition include poor diet and obesity (patients with gout are at high risk for bone spurs).
You may think of the bone spur as your body’s way of trying to compensate for any of the conditions I’ve described by growing a little extra bone. The body doesn’t do a great job of planning where to put it. The little nobs of calcium usually develop around the edges of the vertebrae or along the facing surfaces of the joints. Sometimes the “nobs” resemble small beaks.
Most of the time, bone spurs will not cause problems because they grow in areas where we do not notice them. On occasion, however, they can grow in just the right spot where it will impinge onto a fiber of nerve and possibly compounding a protrusion from a herniated disc. In these cases, you may also be diagnosed with spinal stenosis (narrowing of the spinal passages).
When a bone spur begins to rub against other bones or press on nerves, that’s when you may experience pain, stiffness, tingling, and if left untreated over a long term, numbness and muscle weakness. And that’s when you need to seek treatment.
Conservative treatment for bone spurs begins with non-surgical methods such as medication, anti-inflammatories or muscle relaxant pain medications. Treatment may run for 4 to 6 weeks; however, this is palliative because it provides temporary management and relief for the pain. I will often prescribe physical therapy and muscle strengthening to increase movement, fortify the affected area, and encourage joint strength.
The problem is that bone spurs do not go away on their own. Keep in mind also that bone spurs may be an indication of other issues such as degenerating or herniated discs. Eventually, some surgery may be required.
For patients who visit me at my private practice in Beverly Hills, CA, there are two standard minimally invasive surgical procedures we may consider. The first of these is micro-laminectomy where the surgeon creates a small opening in the bone (lamina of the vertebra) to gain access to the nerve area so that we can make more room for the nerve. We may also consider microdiscectomy where we remove the portion of protruding discs that are compressing nerves. During any of these procedures, we may even shave off bone spurs that are also impinging on the nerve.
Both of these procedures are minimally invasive, facilitated by one or more small incisions to gain access to the affected area with microsurgery tools like a microscope. The process is usually performed on an outpatient basis, which means you’ll be in the doctor’s office for a few hours, then back home for recovery.
If the condition worsens or none of the more conservative approaches is successful, then you and your surgeon will consider more invasive solutions such as artificial disc replacement (ADR).
With ADR, we can reverse the effects of joint overuse and injury by merely replacing a degenerated disc with an artificial one. The procedure is exceptionally advanced, and clinical research data shows a very high success rate in pain reduction and restoring the full natural motion of the spine.
Over the years, having now implanted thousands of artificial discs for both the cervical (neck) and lumbar (lower back) of the spine, I have seen the superior effectiveness of artificial discs. Moreover, I have had many of the same procedures to solve my own long-term spinal problems and can relate with my patients based on my personal experience.
Key to success is that every patient must be assessed individually. Everything depends on a thorough examination of the health of the patient and careful reading of test results. The most crucial factor of all is the benefit to the patient.
That’s how we are greater than better!