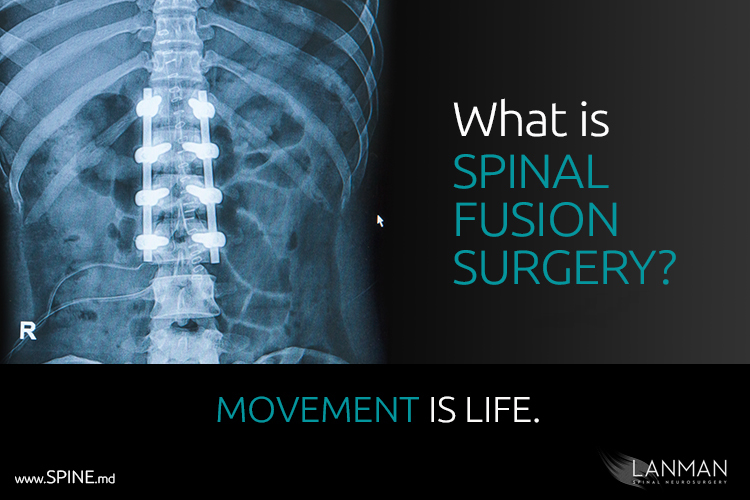
Spinal surgery is a class of surgical procedures that are used to treat patients with spine conditions such as degenerative disc disease, isthmic spondylolisthesis, degenerative spondylolisthesis, and other disorders of the spine.
There are four principle types of spinal surgery: laminectomy, discectomy, spinal fusion, and artificial disc replacement. The specific procedure that a physician will prescribe depends on the diagnosis. When degenerative disc disease is diagnosed, the physician will look for patient discomfort in the form of pain at or near the location where a spinal disc has herniated or ruptured. The patient may also complain about pain and numbness in the extremities; e.g., arms and fingers if the rupture is in the cervical (neck) region of the spine; legs and feet if the trouble is in the lumbar (lower back) region.
For patients that I meet at my practice in Beverly Hills, CA and at Cedar-Sinai Medical Center in Los Angeles, I will often start with conservative non-surgical treatments such as physical therapy combined with pain management. I may also recommend a wellness regimen that adds fitness, nutrition, disease screening, and adjustments to body chemistry. I will recommend surgery if the patient cannot find relief or if the pain increases after 6 to 12 months of non-surgical treatment. For less advanced cases, minimally invasive procedures such as micro-laminectomy or microdiscectomy will likely be proscribed. For more advanced cases, the choice is usually between spinal fusion and artificial disc replacement.
Of the two procedures, artificial disc replacement is preferred primarily because clinical studies show that, unlike fusion, disc replacement preserves the natural range of movement while eliminating the pain generators (e.g., pinched nerves). Artificial discs mimic the form and function of the original discs. Spinal fusion surgery will solve the pain generators as well, however it does so by preventing movement of the vertebral “level” by fusing the two bones together.